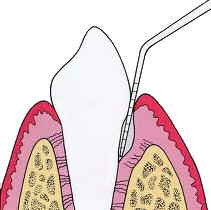
Periodontal Examination & Probing
Gum disease is a health condition that affects over 80% of the population some time in their life. Periodontitis, the most severe type of gum disease, is the main cause of tooth loss.
Periodontal exams for early diagnosis of gum disease can play a critical role in preventing or minimizing the damage to bone and connective tissues around teeth and maintaining your teeth for all your life. Although gum disease in its first stages can be treated easily by just improving daily oral hygiene, many patients with periodontal disease end up at the dentist’s office only when severe damage has already occurred. If gum disease is not diagnosed through periodontal examination before it causes irreversible damage, even extensive periodontal surgery may not be enough to save the patient’s teeth.
The role of the dentist in early diagnosis of periodontal disease
Gum disease at its early stages (gingivitis) gives some warning signs such as red or swollen gums, bleeding and gum recession. But in many cases the symptoms of gum disease are not that intense to alert the patient or they are ignored. The only safe way for the early diagnosis of periodontal disease are the regular visits to the dentist every 6 months.
During a dental check-up the dentist can identify the warning signs of gum disease that may yet be undetectable by the patient. If any symptoms of gingivitis are detected, the dentist will recommend a professional dental cleaning and will give oral hygiene instructions for better control of dental plaque. When more worrying symptoms of periodontitis are present, such as periodontal pockets, pus or loose teeth, the dentist may refer the patient to a periodontist for a more thorough periodontal screening.
A periodontist is a dental specialist who has at least 3 years of extra university training in treating gum disease, and in restoring bone and gum tissue that have been lost because of gum disease.
The Periodontal Exam
A thorough periodontal examination is necessary to assess the health of gums and teeth. A detailed periodontal examination procedure described as Periodontal Screening and Recording (PSR) was previously performed only by periodontists, but today most dentists have included the process as part of a regular dental examination.
The findings will help the dentist to make a precise diagnosis and develop the adequate treatment plan. A periodontal examination should include the following steps and checks:
Medical History - Medication - Habits
The first step of periodontal examination is taking a complete medical and dental history. Many systemic conditions and medications can cause or contribute to gum disease problems. Habits such as smoking and grinding or clenching teeth are also factors increasing the consequences of gum disease. If any of these exists, they should be considered when deciding a treatment plan. Previous incidents of gum disease should also be taken into account.
Evaluation of other risk factors
- Bite or occlusion. The way teeth come together when you bite can affect the health of your teeth. Malocclusion can cause excessive pressure on specific teeth damaging the connective tissues and the bone that support it and worsening the effects of an existing gum disease problem. Crooked teeth can trap food debris and bacteria increasing the risk of periodontal disease.
- Accumulation of plaque on teeth. The amount of dental plaque gives a measure of the quality of the patient’s oral hygiene. Localized accumulation of plaque is an indication of incorrect way of brushing while plaque in interdental spaces is a sign of not flossing.
- Old restorations. Existing restorations such as dental bridges or partial dentures may be sources of bacterial accumulation because they can make it difficult to remove dental plaque if they do not fit properly.
- Missing Teeth. Teeth that have been lost or extracted leave behind an empty space. The adjacent teeth loose their side support and tend to move towards the empty space and become loose. Teeth loss also makes the patient more susceptible to loss of jaw bone. In both cases it becomes easier to bacteria to invade between teeth and gums or bone and cause gum disease.
Physical Examination of the teeth and gums
- Inspection of the gums colour, size, shape, and texture. Reddish, puffy, enlarged or swollen gums are indications of gum disease.
- Tooth Mobility. The dentist will check for loose teeth, by pushing each tooth and observing any movement. Loose teeth is a result of bone support loss that can be caused by periodontal disease or by bruxism.
Periodontal probing - Periodontal Screening and Recording (PSR)
The depth of the periodontal pockets around teeth are the main indicator for the progression of gum disease, and for the level of destruction of periodontal tissues. The process, called periodontal probing, is the main tool used by dentists and periodontists for evaluating the severity of periodontal disease cases. Periodontal probing is the most important part of Periodontal Screening and Recording.
The measurements of periodontal probing are used to calculate either the Periodontal Screen and Recording Index (PSR) which is the system recommended for the early detection of patients with periodontal disease in the US, or the Community Periodontal Index of Treatment Needs (CPITN) which is endorsed by the World Health Organization (WHO).
 A periodontal probe is a long and thin instrument, blunted at the end,
that is calibrated in millimeters (mm), with markings inscribed onto the head of the instrument for measuring pocket depth.
The tip of the instrument is placed with light pressure of 10-20 grams into the gingival sulcus, which is the area between the tooth and the surrounding gums, down to the base of the pocket.
The dentist will gently insert the probe and measure the pocket depth in several (six in PSR) points around each tooth.
A periodontal probe is a long and thin instrument, blunted at the end,
that is calibrated in millimeters (mm), with markings inscribed onto the head of the instrument for measuring pocket depth.
The tip of the instrument is placed with light pressure of 10-20 grams into the gingival sulcus, which is the area between the tooth and the surrounding gums, down to the base of the pocket.
The dentist will gently insert the probe and measure the pocket depth in several (six in PSR) points around each tooth.
In healthy gums, the pocket depth should be less than 3mm. Measured depths over 3mm indicate the presence of gum disease, with the stage of gum disease classified based on the exact depth measured: for depths of 3+ up to 5mm the condition can be classified as mild periodontitis, 5+ up to 6mm as moderate periodontitis and over 6-7mm as severe periodontitis.
The measurements should be carefully recorded, so that the dentist can compare the results after the completion of a gum disease treatment in order to evaluate the success of treatment.
Bleeding during probing. Bleeding of gums during probing is another indicator of gum disease.
Receding gums
Although gum recession is not always caused by gum disease, the dentist will check for receding gums, measuring the distance between the gum margin and the crown of the tooth (cemento-enamel junction).
X-rays - Radiographic Evaluation
X-rays can show the jaw bone condition around the teeth roots. They provide a radiographic image that allows dentists to evaluate the amount and pattern of bone structure loss. If the problem is localized periapical x-rays of the infected tooth may be enough, but in case of severe periodontitis dentists usually request panoramic x-rays in order to have a full image of the condition of all teeth. Radiographs are almost always necessary for a complete evaluation to finalize a diagnosis.
Lumps, lesions or other abnormal changes in the mouth
During a periodontal examination the dentist will also check for any signs that could indicate some form of oral cancer or precancerous condition.
After the Periodontal Exam
Once the periodontal examination is finished, the dentist or the periodontist will evaluate the gathered information about the condition of bone and gum tissues in combination with all the risk factors involved. These will allow the dentist to diagnose the stage of gum disease (gingivitis or early, moderate or advanced periodontitis), in order to develop and recommend a plan for the gum disease treatment.
Other dental health problems that require treatment may also be identified in the process of periodontal examination, such as tooth wear, tooth decay, malocclusion, TMJ disorders, bruxism or cancerous conditions.

