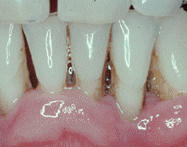
Receding Gums
Receding gums (or gingival recession, or gum recession) is called the condition when the gum tissue surrounding the teeth is lost or pulled away, exposing the roots of the teeth. Gum recession is not directly linked with age but generally it is a more common condition in adults over the age of 40.
Dental health risks related to receding gums
In a healthy mouth the gums (gingiva) along with the periodontal connective tissue (periodontal ligament) surround and support the tooth in the jawbone.
Gum recession usually involves a significant loss of these protective tissues. The gum line is pulled away towards the root allowing a larger part of the tooth to be visible and in contact with the mouth’s environment.
Healthy gums fit firmly against teeth covering the root area. The immediate result of receding gums is the exposure of the root and the loss of attachment between the gums and the tooth.
- Tooth decay. The root of the tooth is covered by cementum which is a hard material but not as hard as the enamel that covers the crown of the tooth. Cementum is also thinner than the enamel. The exposed part of the root surface is much more susceptible to tooth decay and cavities, due to the limited protection of the cementum.
- Periodontal disease. The gums do not attach firmly on the tooth, forming a periodontal pocket and allowing mouth bacteria to enter and grow in the space between them. The dental plaque and food debris accumulated in the periodontal pockets are difficult to brush and floss away. If the growth of dental plaque bacteria is not controlled, the condition might progress to the much more serious periodontal disease (periodontitis), resulting in jaw bone and tooth loss.
- Appearance. Besides the medical complications there is also a cosmetic one. Receding gums may damage the appearance of your smile making it unattractive.
Symptoms of Receding Gums
Gum recession is not something that happens overnight. In most cases, receding of gums is a progressive procedure that happens gradually from day to day over the years. That explains the fact that it is common over the age of 40. Because the changes in the condition of the gums from one day to another are minimal, we get used to the gums appearance and do not notice the changes over longer periods of time. Receding gums may remain unnoticed until someone else talks to us about it or until the condition starts to cause other problems.
The following signs and symptoms may indicate gum recession:
- Sensitive teeth. Teeth become sensitive to hot and cold or to sweet, sour or spicy foods. If the cementum covering the root is not protected any more by the gums it is easily abraded exposing the dentin tubules to external stimuli.
- Teeth may also appear longer than normal (more part of them is visible if gums are receding).
- The roots of the tooth are exposed and visible.
- The tooth feels notched at the gum line
- Change in the tooth’s color (due to the color difference between enamel and cementum)
- Spaces between teeth seem to grow (actually the space is the same but it seems larger because the gums do not fill it any more).
- Cavities below the gum line
If the gum recession is causes by gingivitis, the following symptoms may also be present :
- Puffy, red or swollen (inflamed) gums
- Gum bleeding while brushing or flossing
- Bad breath (halitosis)
- In some cases, it is the treatment of gingivitis that reveals a receeding gums problem, that was previously masked by the gums swelling.
Diagnosis of Receding Gums
The dentist diagnoses gingival recession by a simple visual examination of the teeth. What is more important is the diagnosis of the cause of receeding gums.
If the problem is located on only some teeth, usually the front teeth, it is an indication that way of brushing and abrasion is the cause of receding gums. The dentist will also examine if the bite alignment (occlusion) or tooth grinding (bruxism) is causing gingival recession to the teeth involved.
If all teeth have receding gums, it is more likely that gum disease should be blamed. A periodontal screening examination including x-rays and periodontal probe measurements is needed to diagnose the extent of periodontal disease and possible damages.
Causes and Risk Factors of Receding Gums
Gum recession occurs because of damage to the gum tissue. The two common causes of receeding gums are improper toothbrushing and gingivitis / periodontitis, or the combination of both.
- Gum disease is the main cause of receding gums. If the dental plaque is not removed by daily oral hygiene, toxins produced from the bacterial metabolism irritate and inflame the gums causing gum disease. Gums swelling and bleeding are common signs of the disease. The inflammation starts to destroy the gingival and connective tissues, causing the gums to separate from the tooth and retreat towards the roots of the teeth. Actually, it is not only the bacteria that cause the tissue damage and periodontal gum recession, but also the body’s immune system effort to fight the dental plaque bacteria.
- Aggressive tooth brushing / Hard toothbrush / Wrong way of brushing or flossing. They all can damage the thin gum tissue causing it to break down.
The improper mechanical use of the toothbrush is a key cause for gum recession.
o Increased pressure on the toothbrush or dental floss will only harm gingival tissue without increasing the cleaning action of brushing or flossing.
o The same applies to the use of a hard toothbrush that will make things worse if any other reason co insists.
o Wrong way of brushing such as making large horizontal movements over the teeth is damaging not only the gums but it is also abrading the cementum exposing the dentin and causing sensitive teeth. - Age can also play a role in receeding gums, especially in women. Damage to the gums caused by improper brushing is progressively accumulated over the years, resulting in receding gum line. Older women after menopause can suffer from osteoporosis. Loss of mass from alveolar bone that is supporting the gums and teeth can cause gingival recession.
Other possible causes of receding gums include:
- Poor oral hygiene. Inadequate brushing or flossing may not directly causing gum recession, but it allows the overgrowth of mouth bacteria and the accumulation of dental plaque, causing gingivitis and potentially periodontitis.
- Mouth trauma or injury could make the gums to recede. Other forms of trauma, such as oral piercing that rub against gum tissue can also cause the gums to recede.
- Occlusion problems / Misaligned or crooked teeth. Receding gums may occur when teeth are crooked or fillings and crowns are placed without properly balancing the bite. If the teeth do not come together properly, excessive forces are placed on certain parts of the teeth and that may cause trauma to the bone and gums.
- Grinding or/and clenching teeth is also putting teeth under excessive pressure, sometimes resulting in gum recession.
Prevention of Gingival Recession
Gum recession is a condition that can be easily prevented by good daily oral hygiene habits.
- Brush your teeth at least twice a day and floss at least once to prevent dental plaque and gum disease.
- Visit your dentist for regular dental cleanings and examination every 6 months.
- Use a good quality soft toothbrush with small head and rounded bristles. Do not put excessive pressure on the toothbrush when brushing.
- A pressure-sensitive toothbrush such as the new Oral-B Triumph with SmartGuide (that shuts off automatically when too much pressure is applied to the teeth) can also help reduce the risk of gingival recession.
- Ask your dentist to show you the correct way of brushing your teeth. Brushing will help you to stop receding gums only if done properly.
Treatment for Receding Gums
The first step of the treatment for receding gums involves the elimination of the underlying causes of the problem.
- Practicing good oral hygiene is usually enough in the majority of cases, either caused of improper toothbrushing or by gum disease, to provide natural cure for receding gums. If oral hygiene can not reverse receding gums, further treatment may be needed. Depending on the severity and the causes of receding gums, treatment can be surgical or non-surgical. Depending on the kind of the appropriate treatment for receding gums, it may be performed by a dentist, an oral and maxillofacial surgeon, an orthodontist or a periodontist.
non-surgical treatments for gum recession
- Desensitizing toothpastes. There are several toothpastes against tooth sensitivity, with agents such as sodium chloride or potassium salts that block the creation or transmission of the pain sensation.
- Desensitizing agents. Fluoride gels, resins and other desensitizing agents can be applied by the dentist directly to the exposed areas of the teeth and roots, providing immediate sensitivity pain relief.
- Resin-bonded restorations or other types of fillings can be placed over the worn areas along the necks of the teeth.
- Tooth scaling and Root planing. Professional deep cleaning of the tooth surfaces below the gum line may be required to treat gum disease and stop the gum recession.
- Correction of malocclusion and treatment of tooth grinding and clenching.
Surgical treatment for receding gums
Severe cases of receeding gums require surgical treatment to be performed, usually by a periodontist, who is a specialist in treatment of the gum diseases.
- Soft tissue graft is a procedure also known as gum graft surgery that covers the exposed root surface. If the gums are badly damaged, the only treatment option to restore receded gums is the use of a soft tissue graft from another part of the mouth. The piece of gum tissue that will be used as graft can be taken from around an adjacent tooth or from the palate of the mouth. The soft tissue graft is then sutured to the damaged area around the roots. Soft tissue graft is a gum tissue regeneration procedure that replaces the lost or receded gum tissue, covers the sensitive roots and protects the patient from further gums recession.
![]() The cost involved with dental treatments can be significant and many patients may not afford it if they are not covered by their dental insurance.
Learn how to choose a dental insurance plan that will provide the best dental treatment to you and your family.
The cost involved with dental treatments can be significant and many patients may not afford it if they are not covered by their dental insurance.
Learn how to choose a dental insurance plan that will provide the best dental treatment to you and your family.

